La celiachia è una delle intolleranze più diffuse al mondo. In alcuni paesi la percentuale della popolazione colpita dalla malattia raggiunge 1%, come mostrano i risultati di alcuni screening.
Secondo i dati riportati sulla relazione annuale al Parlamento sulla celiachia anno 2016 in Italia risultano 198.427 celiaci, più di 15.000 rispetto al 2015, di cui il 46 % è concentrato al Nord, il 21 % al Centro, il 22 % al Sud e l’11 % nelle Isole. La regione dove risiedono più celiaci risulta la Lombardia, con 37.907 soggetti, seguita dal Lazio con 19.325 e dalla Campania con 18.720.
Il Lazio è anche la seconda regione per numero di nuove diagnosi, con 1.548 celiaci neo-diagnosticati, dopo la Lombardia con 5.499.
Per molto tempo la celiachia è stata considerata una rara patologia infantile. 20 anni fa la sua prevalenza oscillava ancora tra 1 : 1.000 e 1 : 2.000. Questi dati si basano sul manifestarsi di patologie conclamate e tipiche forme di celiachia. La scoperta di varie tipologie di anticorpi specifici per la celiachia e gli screening degli ultimi anni hanno dimostrato che la celiachia è molto più diffusa di quanto si creda. Le donne hanno il 50 per cento di probabilità in più di ammalarsi di celiachia rispetto agli uomini. In alcuni paesi è stata descritta una prevalenza della celiachia che oscilla tra 1 : 100 e 1 : 500. Ciò significa che l’un per cento della popolazione è affetto da celiachia.
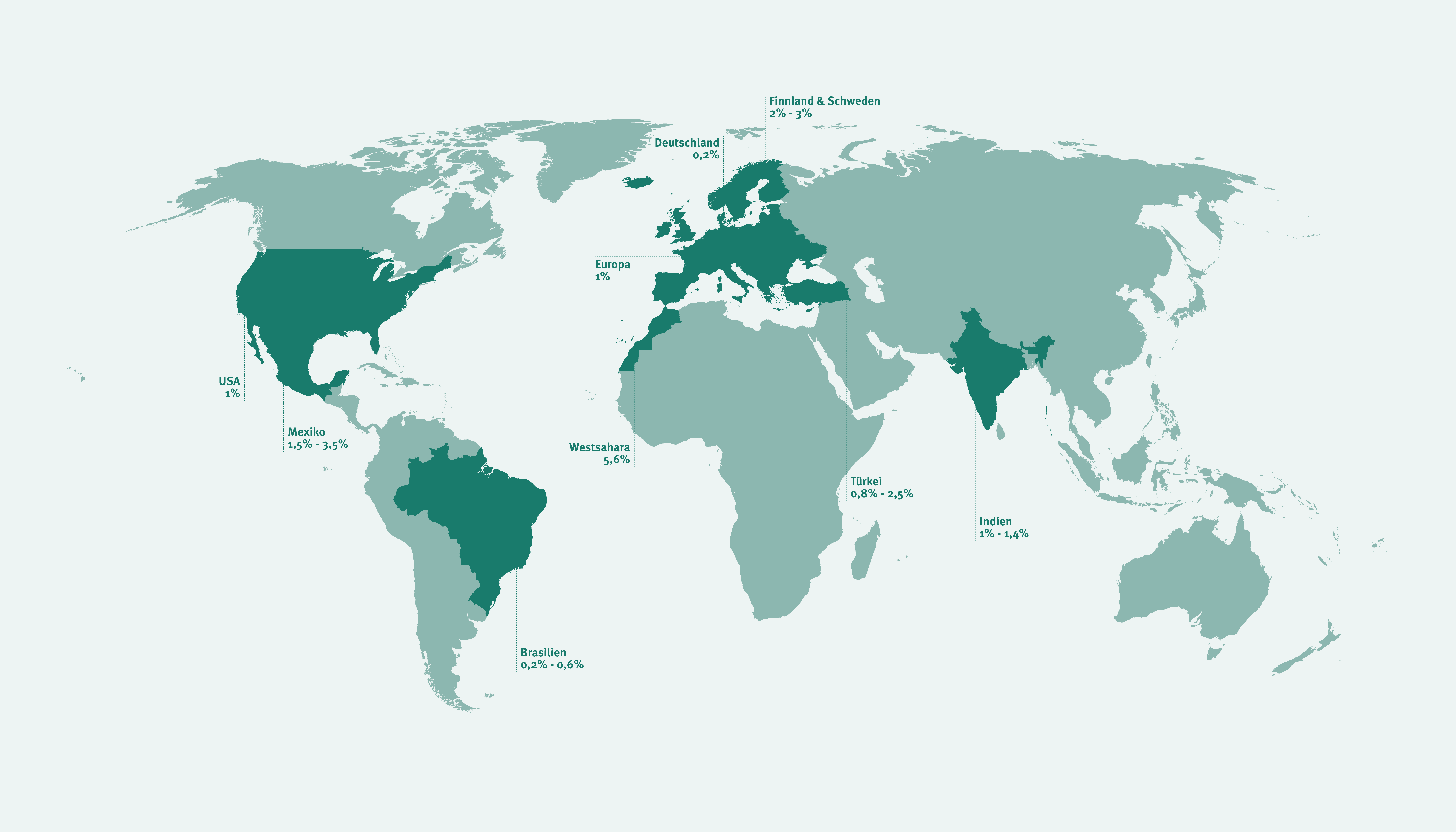
Planisfero della celiachia
Uno studio pubblicato nel 2014 mostra che l’incidenza della celiachia è quintuplicata negli ultimi 25 anni. Tra le regioni caratterizzate da una prevalenza che raggiunge l’un per cento della popolazione vi sono l’Europa e gli Stati Uniti, dove l’alimentazione tradizionalmente si basa su alimenti ricchi di glutine. Una frequenza simile a quella europea è stata riscontrata anche nelle popolazioni dell’Africa settentrionale, del Vicino Oriente e dell’India.

Iceberg della celiachia
La maggior parte dei casi di celiachia sono asintomatici, non mostrano alcun decorso tipico e restano a lungo non diagnosticati. Il lasso di tempo che intercorre tra il manifestarsi dei primi sintomi e la diagnosi della celiachia può estendersi a sette anni. È stato calcolato che a un caso diagnosticato corrispondono da tre a cinque casi non diagnosticati. Per questo motivo si parla spesso di “iceberg della celiachia”.
Picco di età della celiachia
Ormai accade sempre più di frequente che la celiachia sia diagnosticata in età adulta. Se prima del 1981 l’età media dei pazienti alla prima diagnosi si aggirava intorno ai 30 anni, oggi è compresa tra i 40 e i 45 anni. Con l’avanzare dell’età si è modificato anche il quadro clinico della patologia: molti pazienti a cui la malattia è stata diagnosticata in età adulta, presentano i sintomi extra intestinali propri di una celiachia sintomatica .
Fonti
- Catassi C., Gatti S., Fasano A. The New Epidemiology of Celiac Disease Journal of Pediatric Gastroenterology & Nutrition, July 2014 Volume 59.
- Mustalahti et al., The prevalence of celiac disease in Europe: Results of a centralized, international mass screening project. Annals of Medicine 2010 Dec;42(8):587-95.
